On January 14, I published my first medical update of 2021, which you can access here, if you missed it. Basically, the cliff’s notes version is this: pesky met in my pelvis won’t die, first biopsy attempt did not show anything actionable, and we’re trying to figure out what to do next.
One major ah-ha moment for me this past week was when I was able to speak directly with the cryoablation expert at the Duke Bone Mets Clinic, Dr. Sag. My husband and were very impressed by his empathy, caring, and ability to translate complicated medical concepts into plain, understandable language. To me, that’s the true test of being an expert — being able to translate their expertise into plain language. The light that he turned on was about the question of pain. I’ve been telling everyone that the pesky met is asymptomatic; however, some of the pain I’ve been attributing to the mets in my hips and the surgical changes from inserting the titanium rods inside my femurs, is almost certainly attributable to the pesky met per that discussion.
Understanding that I am experiencing some symptoms from the pesky met was a pretty huge ah-ha moment and something that definitely has changed some of the urgency of addressing the pesky met. As my medical oncologist said, it’s always good to get confirmation that we’re on the right track and need to deal with it rather than just watching it.
Also last week, on inauguration day, I underwent a CT planning session for SBRT and, on Friday, consulted with the interventional radiology experts as recommended by my medical oncologist to get better information and to be able to compare apples to apples when selecting the best next step for me. I haven’t had radiation since 2017 when, just after my leg surgery, the rods inside my femurs were radiated along with L2, where a large lesion was threatening to collapse that vertebrae. I vaguely remember the planning session and undergoing radiation, but I was still in the haze of being newly diagnosed and was still using a walker to get around, so I’ve forgotten a lot.
So different this time!
For the planning session, I had to completely disrobe and then they used some strategically placed pieces of cloth to preserve my modesty (for those of you who are cancer patients, you are probably laughing here since there is really no modesty in cancer treatment). Then, I laid down on the part of the CT machine that would slide in and out or up and down, whichever way they needed me to go — its usually hard and cold. However, this time, the place where I was laying had a special bag full of pellets that look like styrofoam. Once I had laid down, they confirmed I was straight, and the air was then pumped out of the bag I was laying on. By doing so, there is now a bag shaped imprint exactly like my body that I will lay on during the three (3) session of radiation treatment, if we indeed decide to proceed in that direction. Then, a large plastic sheet was draped over me and connected to the bag I was laying on by tape and other sticky areas after they had put a tube over me — no, it wasn’t duct tape, although it looked like it! Once a seal was obtained, the tube was activated to suck all the air out of the sandwich with me inside (you can see the tube covered with white cushioning in the pictures below).
In essence, I was shrink wrapped to the table. My entire body was compressed inside the bag molded to my body and covered by plastic. The purpose of this process is to keep me 100% entirely still during the radiation treatments and boy is it good at that — I couldn’t move a muscle even if I wanted to and it wasn’t super easy to breathe.
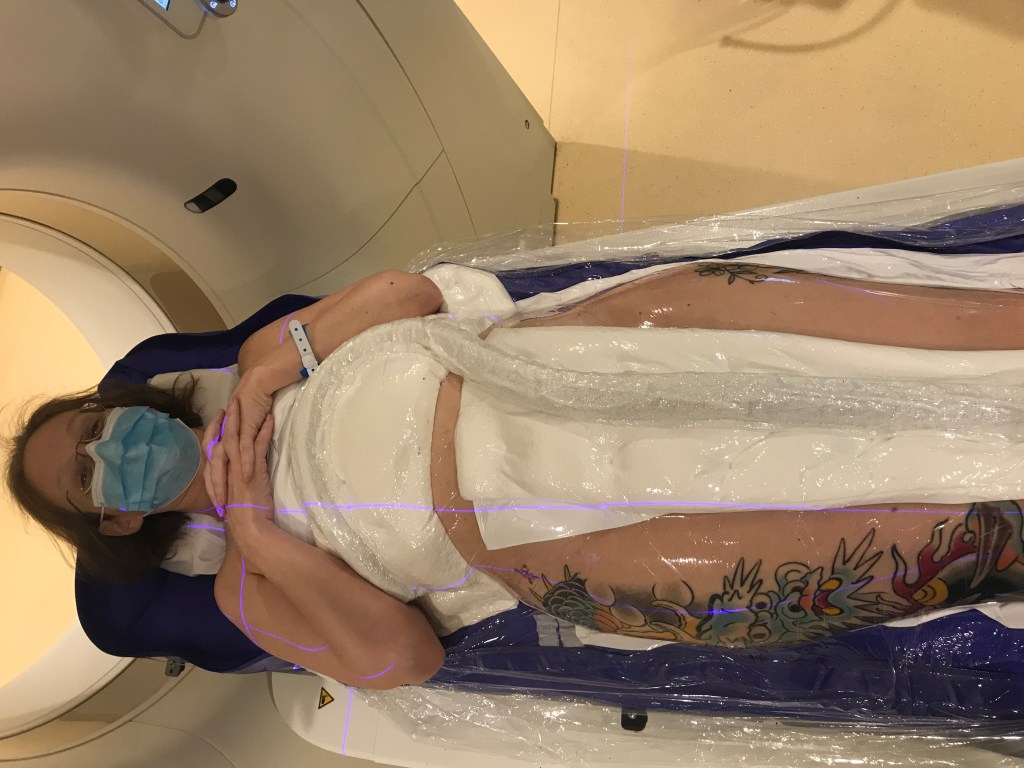

The techs only needed to give me one more radiation tattoo since they can use the other tattoos I got to cover the scars of my leg surgery to ensure that I’m in the same place each time. There is literally a grid of lasers that is embedded in the room where the radiation occurs and they use the bio markers or tattoos to ensure that I’m in the same exact place each time. The radiation physicist paid us a visit during this session to check to give the thumbs up.
When I’m nervous or feeling unsettled or there is too much seriousness, I tend to try to lighten the mood by cracking jokes. Ok, so I’m not that funny, but I can usually get a few smiles and things feel a little more comfortable. My feelings of anxiety are exacerbated when something is happening to me, to my body, and no one is explaining what they are doing or why. I’ve found that trying to be funny and failing usually reminds the people in the room that I’m a person and I don’t have to ask “what’s happening now” or “why are you doing this” too many times, which some people have interpreted as interference in the past.
Just one of my coping mechanisms that sometimes works and often just makes me sound a little like an unfunny person trying to be funny. Clearly the techs were humoring me by chuckling at my efforts, but I could not for the life of me get that physicist to crack a smile. Guess I’ll have to brush up on jokes that would resonate with a physicist — if any of you know some, feel free to include that in the comments or send me a message.
During the consult last Friday with the interventional radiology experts, we went over the need to get another biopsy (I can’t do radiation without a biopsy that shows cancer), the potential of using cryoablation to deal with the pesky met, and attempting to compare the options (cryoablation versus SBRT radiation) head to head as much as possible. I’ve not yet encountered a situation like this, where there are small (10% or lower) differences between two potential options and there isn’t a clear best option. The way I deal with decisions usually is to obtain as much concrete, objective information as possible to be able to literally list out the pros and cons — this applies to medical decisions as well as anything else.
The emotional impacts of procedures is a hard thing to quantify and are usually the last thing I enter into an equation, partly because it is truly difficult to quantify, and yet there is an emotional element to this decision. It’s hard to describe how heavy this decision weighs on me and how hard it is to see a clear path through all of the options and risks and side effects and time and different offices. As much as I am trying to make this an objective though process, I’m still sorting out how I feel as well and that can be truly heavy.
Stay tuned for the decisions and how the treatment goes!

Thank you for sharing your experience here. What a kind and generous thing to do. Best wishes.
LikeLiked by 2 people
Thank you so much for sharing your experiences.
LikeLiked by 1 person
I ready enjoy your words of encouragement. I learned laughter is the best medicine. I thank you for sharing your experiences. I pray the experts will comes up with a cure that will saves many lives.
LikeLiked by 1 person
There’s bound to be some physicist light bulb jokes out there, that perhaps might elicit a smile.
LikeLiked by 1 person
Yes, so true! Lol
LikeLike
Praying God gives you clarity for the decisions ahead. 🙏❤️
LikeLiked by 1 person
Thank you. It’s been a doozy!!
LikeLike
You really made me laugh this time, because when I saw the picture, I thought to myself… How in the world did she convince somebody to climb up and take a picture from up high!? How did she even get the nerve to ask. And what did she say? Two paragraphs later you were telling us how you finally asked somebody to take a picture for the first time, and I cracked up. 😂
I also cracked up about the modesty thing. I’ve had medical issues my entire life, so modesty is really just not a thing for me, nor is being jabbed over and over again. There are certain medical experience is that once you have been through them, you just don’t care anymore. But they did a good job! And we got to see your tat!
I see we also share some thing else in common. Cracking jokes to make things less uncomfortable. I do this exact thing. And I’ve tried to figure out why. Even in an ambulance, I have said things that have made the driver start cracking up from the front. 😂
LikeLiked by 2 people
Lol. I’ve seen other people ask to have pictures taken and always thought, eventually I’ll have the nerve to ask. And I just couldn’t help it this time because it was such a process!! ❤️
LikeLiked by 1 person
You looked like a beautiful, Egyptian/Grecian princess with the gown thing going on. That sounds like an exhausting day. I hope you treated yourself afterwards.
LikeLiked by 1 person
Definitely! Thanks!
LikeLiked by 1 person
You do a great job of describing the experience in a way to reduce the anxiety of others who might be facing the same thing. Adding the picture is an extra bonus because we always conjure up the worst in our heads. You’ll never know how many lives you’ve impacted with your words. Just wish you didn’t have to experience all this….here’s to sending that ‘pesky met’ packing!! Big hugs!!
LikeLiked by 1 person
Oh, yes, I always conjure the worst possible thing when left to my own devices!! Thank you, my friend. 🙂
LikeLike
Thank you fir sharing. Is this standard case (ha ha – what’s standard with Cancer?). I also try humor, but sarcastic Junie. I need it!
LikeLiked by 1 person
I’ve heard from others doing SBRT that they didn’t get shrink wrapped so I’m not sure. Perhaps it’s a thing my doc prefers? Hard to know.
LikeLike
I also thank you for sharing your experience, and I have to say, I love your tattoos!
LikeLiked by 1 person
Thanks!
LikeLike
Reblogged this on By the Mighty Mumford.
LikeLiked by 1 person
Thank you!!
LikeLiked by 1 person
YOU ARE WELCOME
LikeLiked by 1 person
I just shared this post with a blogging friend, Sue Vincent, who has been diagnosed with terminal lung cancer. You are such an inspiration, Abigail. Your options seem so grim, yet there you are cracking jokes. That is what I try to do, too, and most of the time I get the same results you do and even some “Huhs?” But it is a postivie way of coping with a horrible situation. Nice tats, BTW. I hope you have a better week. Lots of love and prayers.
LikeLiked by 1 person
Thank you!! I think we have a choice at times at how to approach a difficult situation. I am not always able to crack jokes and see the positive side of things; at the same time, when I focus my energy on finding the silver linings rather than wallowing in the negatives, i usually have a better experience. Our minds are powerful things. That being said, I also rage and rail against all the negative parts of dealing with a terminal illness and a medical system that regularly and consistently takes away our basic humanity. Thanks for commenting and for sharing!
LikeLiked by 1 person
It’s the least I can do, Abigail. You know the old adage, “But for the grace of God, there go I.” Whether any of us want to admit it or not, it is true. Who knows why a beautiful, brilliant young mother should have to suffer as you do. But you are in the middle of it, and there is not much you or anyone else can do but pray and be there and be sad that it is happening to you. Lots of love.
LikeLiked by 1 person
❤️
LikeLike
Abigail
You are in my thoughts and prayers. I’m the very lucky six-year pancreatic survivor who blogs at https://survivingcancerembracinglife.com. You are truly an inspiration. Thank you for sharing. And being so open.
All the best.
Joel
LikeLiked by 1 person
Thank you.
LikeLike
After an ordeal like that one deserves pampering for a thousand years, well for a little while anyway. I hope you had such a treat afterwards.
Oh, and your tattoo looks amazing under the plastic, likened to how awesome tattoos look when wet.
Medical stuff really sucks, that’s for sure.
Andro
LikeLiked by 1 person
Thanks!! Yes, medical stuff is not easy. The radiation appears to have worked and the pesky met is correctly dying.
LikeLike